The case that tears at heart strings
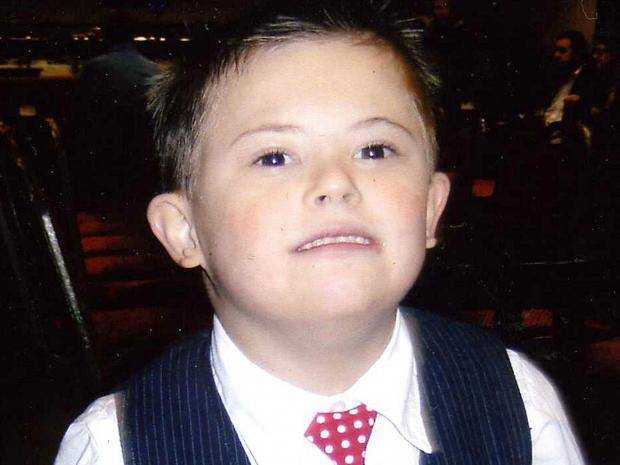
There is currently a frenzied backlash amongst doctors in the UK against the striking off from the medical register of Dr Hadiza Bawa-Garba, a paediatric registrar who was convicted of gross negligence manslaughter over the death of Jack Adcock (pictured above.)
The young boy was treated at Leicester Royal Infirmary by doctor Bawa-Garba before tragically dying of sepsis. Initially following her conviction she was suspended for a period of 12 months, but the GMC (General medical council – a body which regulates doctors in the UK) challenged this decision and succeeded in striking Dr Bawa-Garba from the medical register, meaning she will not be able to practice in the UK. This has prompted outrage in the medical community, with over £300000 being raised by crowdfunding for Dr Bawa-Garba’s appeal.
Why has the medical community reacted this way?
Well, for a number of reasons;
- It is a scary fact that most doctors at one time or another have, or most certainly will, underestimate how sick a patient is. It is easy to empathise with Dr. Bawa-Garba on this point, sepsis after all is the silent killer.
- All doctors can relate to being over stretched, and working in dangerous conditions (especially during the winter months,) almost daily. You will always be treating too many patients, or there will be too long a waiting time, or you’ll be dealing with IT from the 80s that constantly crashes (as was the case here.)
- It raises the question, to what extent can doctors be held accountable after a mistake? They are, after all, all human, and certainly Dr. Bawa-Garba had no intention to commit harm and was at the time doing her best to do a good job on the day in question. But was it the best she could have done for Jack?
The above leads to a scary realisation for doctors, no matter how hard you work, how good you are, one mistake can bring you down.
But what about the flip side?
But what about Jack, and his family, are they not entitled to some justice? After all, there were plenty of signs that Jack was indeed, very ill, and these weren’t acted upon.
- For starters, Jack was brought in requiring a small amount of oxygen to help with his breathing. Now this can be easily missed, but points to an underlying issue that requires further scrutiny. Dr. Bawa-Garba did ask for a chest x-ray but due to pressures this was not performed for a few hours, and the results seen a few hours after that. Some doctors, however, seeing a child requiring oxygen, a mother who is convinced that the child is sick, with a background of Down’s Syndrome and clinical signs of infection would have started antibiotics right away. This could have saved Jack’s life.
- An initial blood test showed a very high lactate. This is a marker in the blood that basically shows that your body is not coping well with something. It was high enough that it should have warranted immediate repeating and commencement of antibiotics and fluids. Dr. Bawa-Garba noted the lactate and did convey it to a superior who suggested that the test be repeated. This was not done I am assuming due to time pressures. Again had this been done, it might have saved Jack’s life
There were many other errors attributed to Dr Bawa-Garba, however these in my mind were smaller and not what could have been turning points for her – though others might disagree. The above I feel are the biggest areas which could have triggered the commencement of antibiotics and possible subsequent survival of Jack.
So, the debate…
Jeremy Hunt has said that he is perplexed by The GMC taking upon itself to appeal Dr Bawa-Garba’s suspension. In a way I would say that I agree. The GMC has an inconsistent history in how it treats doctors and there are some allegations of racism, which though I am sure are unconscious I believe may be true.
Doctor’s should feel that they are protected legally when they make what during a long career, will be inevitable errors. Some of these may lead to deaths but I am afraid that this is a hazard of the industry. The question here is whether this truly was negligence as opposed to mistakes that any other doctor could have made.
On this point I am not so sure, I would like to think that most doctors seeing a lactate of greater than ten would know that this requires immediate action, whether you are busy or not. If you are too busy to address this then it would require drafting in of help, of which there are other teams in the hospital. However, it is true that Dr. Bawa-Garba was truly swamped and may have been overloaded with information sufficiently to miss the significance of the test. I would argue however, that if you are working under these extremes you have to notify a senior. Patients in this scenario are being placed at unacceptable risk.
So in conclusion, do I feel that Dr Bawa-Garba should be struck off from the medical register? The GMC maintains that the public would lose faith in the profession were she not to be. Nicola Adcock, Jack’s mother, asks the simple question – “would you want this doctor treating your child?” Regrettably, my answer is no, I would not.